

Maternal and Child Health Integrated Program (MCHIP)
About
The USAID Bureau for Global Health’s flagship Maternal and Child Health Integrated Program (MCHIP) worked in more than 50 developing countries in Africa, Asia, Latin America and the Caribbean to improve the health of women and their families. MCHIP supported programming in maternal, newborn and child health, immunization, family planning, nutrition, malaria and HIV/AIDS, and encouraged opportunities for integration of programs and services when feasible.
MCHIP addressed the barriers to accessing and using key evidence-based interventions across the life stages—from pre-pregnancy to age 5—by linking communities, primary health facilities and hospitals. By helping countries identify and focus on those innovations that will save lives, MCHIP supported delivery of evidence-based interventions through strengthening government health systems, nongovernmental organizations and other local partners.
In June 2014, USAID announced MCHIP’s successor program, the Maternal and Child Survival Program. Visit this flagship program, working to end preventable child and maternal deaths, at www.mcsprogram.org.
Impact
MCHIP activities contributed to global reductions in maternal and child deaths, and improved the health of women (from planning a family through pregnancy and delivery) and their children (from infancy through childhood). At the household, community and hospital levels, MCHIP implemented and worked to scale up high-impact interventions.

Sustaining these achievements requires national policies, training and contributions to global learning:
– Across MCHIP countries, USG-supported training programs graduated nearly 308,000* participants.
– Over the life of the project, 182 national policies were drafted with USG support.
* Actual total for life of project is 307,759 total training participants.
Interventions
MCHIP supported programming in maternal, newborn and child health, immunization, family planning, malaria and HIV/AIDS, and strongly encouraged opportunities for integration. Cross-cutting technical areas included water, sanitation, hygiene, urban health, and health systems strengthening. MCHIP presented a vehicle in which the whole is greater than the sum of individual parts, enabling the Program to respond to the need for a more integrated approach to services while taking into account epidemiology, health system capacity, efficacy, coverage, cost, cultural acceptability and other factors.
Country Programs
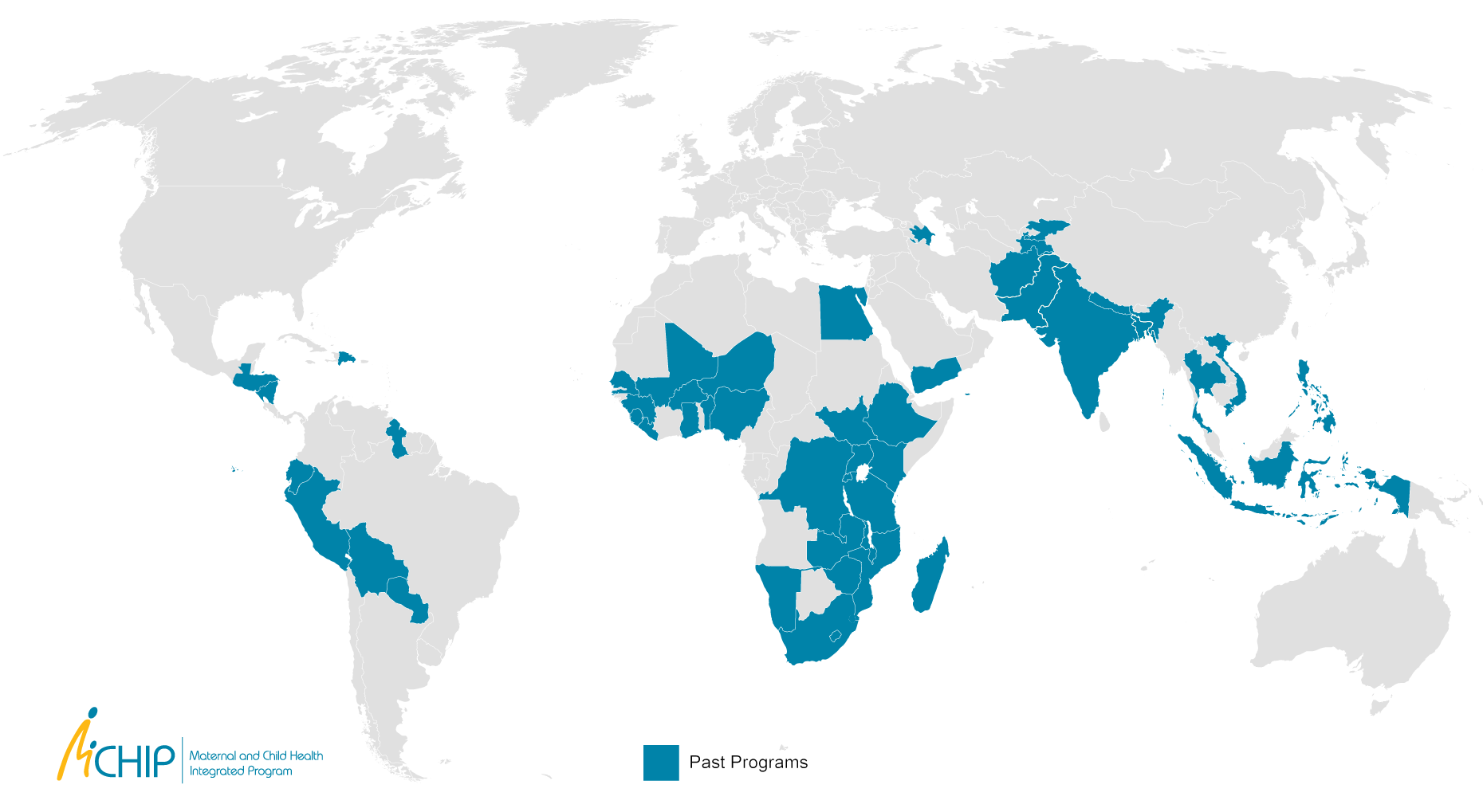
Programs
- Bangladesh
- Bolivia
- Burkina Faso
- Burma
- Democratic Republic of Congo
- Dominican Republic
- Egypt
- Ethiopia
- Ghana
- Guinea
- Guyana
- India
- Indonesia
- Kenya
- Kyrgyzstan
- Lesotho
- Liberia
- Madagascar
- Malawi
- Mali
- Namibia
- Mozambique
- Nepal
- Nigeria
- Pakistan
- Paraguay
- Philippines
- Republic of South Sudan
- Rwanda
- Senegal
- South Africa
- Swaziland
- Tajikistan
- Tanzania
- Timor-Leste
- Uganda
- Ukraine
- Vietnam
- Yemen
- Zambia
- Zimbabwe
Technical assistance was also provided in:
- Afghanistan
- Benin
- Burundi
- El Salvador
- Guatemala
- Honduras
- Nicaragua
- Niger
- Peru
- Sierra Leone
Resources & Learning
Although the strategies for implementation varied widely from country to country, dependent on contextual factors such as the strength of the health system, the relationship with the government, cultural factors, geography, etc., several key themes, were critical for success, regardless of region or intervention. These resources explore learning on four key themes – scale up, community level activities, quality of service provision, and equity – from the broad experiences of MCHIP, as well as the broader reproductive, maternal, newborn and child health community.
Of the low- and middle-income countries that have achieved the greatest declines in under-five mortality since 1990, strong community-based programs that rely on community-level providers is a common feature. And existing and growing evidence speaks to the positive contributions that community health workers (CHWs) are making to these improved health outcomes.
MCHIP understood that these facts—and the estimated worldwide shortage of 4.3 million health workers—meant that well-functioning CHW programs were key to improving the health of vulnerable populations. As a result, the Program worked to strengthen the capacity of health systems to engage communities and to build strong systems of service delivery outside of health facilities that have the ability to reach those that were not yet being reached by essential health services.







